-
SILICON VALLEY: Indian-origin executive named CEO of Microsoft Gaming - March 5, 2026
-
WASHINGTON: Indian-American lawyer at center of Trump’s biggest legal setback - March 4, 2026
-
TEXAS: ’15 of my cousins came here on H-1B’ - March 3, 2026
-
NEW YORK: Indian-origin doctor shares mother’s immigrant success journey in US - March 2, 2026
-
ARIZONA: Indian-origin scientist wins Arizona State University’s top Science Prize - March 1, 2026
-
WASHINGTON: Balaji Krishnamoorthy becoming Uber CFO amid ongoing visa row - February 28, 2026
-
LUCKNOW: Prime Minister Narendra Modi on HCL-Foxconn chip facility in UP - February 27, 2026
-
WASHINGTON: 55% Indian Americans Disapprove Of Trump’s India Policies: Survey - February 26, 2026
-
WASHINGTON: Trump Praises Indian American Harmeet Dhillon Amid Harvard Case - February 26, 2026
-
MUMBAI: Ranbir Kapoor to set up new RK Studios - February 25, 2026
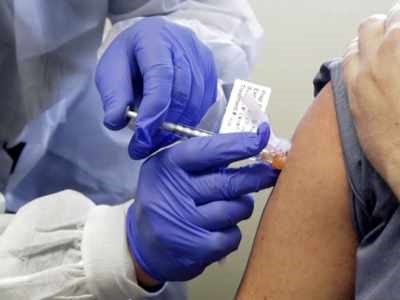
BOSTON: Study sheds light on critical windows in pregnancy for Covid-19 vaccination
BOSTON:
Scientists have found evidence of lower than expected transfer of protective
antibodies against the novel coronavirus via the placenta from mothers who are
infected in the third trimester, findings that shed light on critical windows
in pregnancy that may be most desirable for vaccination.
According to the researchers, including those from Massachusetts General
Hospital (MGH) in the US, the findings may be explained by a process where the
carbohydrate molecules in the body alter antibodies after they are produced.
They explained that altered
attachments of carbohydrates to the coronavirus-specific antibodies — a
process called glycosylation — may be to blame for the reduced transfer from
mother to fetus.
In the study, published in the journal Cell, the scientists compared maternal
antibodies against the flu (influenza), whooping cough (pertussis), and the
novel coronavirus — SARS-CoV-2 — and how these antibodies transferred across
the placenta.
They found that influenza- and pertussis-specific antibodies were actively
transferred in a relatively normal fashion.
In contrast, the researchers said the transfer of SARS-CoV-2-specific
antibodies to the baby was not only significantly reduced, but the antibodies
transferred were less functional than those against influenza.
According to the scientists, the reduced transfer was only observed in third
trimester infection.
The study found that carbohydrate attachments on SARS-CoV-2-specific antibodies
in maternal blood were different than those seen on influenza- and
pertussis-specific antibodies.
The researchers believe this carbohydrate pattern may cause the COVID-specific
antibodies to be “stuck” in the maternal circulation, rather than
transferred across the placenta via placental antibody receptors.
However, the scientists said some increases in total maternal antibodies
induced by viral infection helped to partially overcome the problem and
facilitate the transfer of some functional antibodies from mother to fetus.
A higher placental expression of a receptor which attracts the carbohydrate
pattern on the SARS-CoV-2-specific antibodies also helped, the study noted.
Based on the analysis, the scientists said some of the antibodies that
transferred the best were also the most functional, activating the immune
system’s natural killer cells that could help the newborn fight the virus if
exposed.
The researchers believe the findings have implications for the design of new
vaccine candidates against SARS-CoV-2 for pregnant women.
“Vaccine regimens able to drive high levels of the COVID-specific
antibodies with glycosylation patterns favoured by the placenta for selective
transfer to the fetus may lead to better neonatal and infant protection,”
says study co-author Andrea Edlow, a maternal-fetal medicine specialist at
Massachusetts General Hospital.
The scientists said the study results may point to critical windows in
pregnancy that may be most desirable for vaccination to optimise protection for
both the mother and her infant.